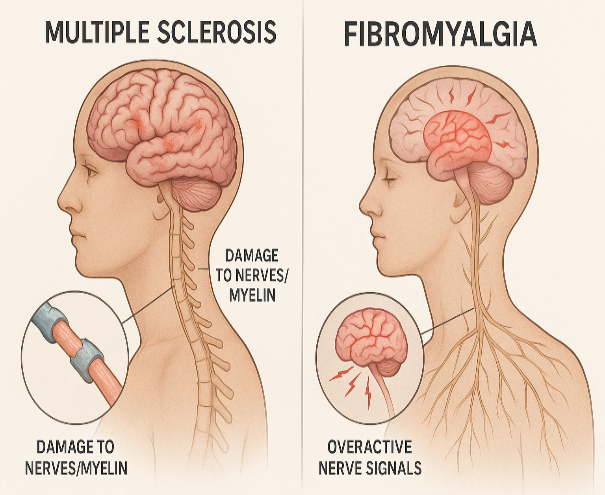
Multiple sclerosis and fibromyalgia both involve the nervous system and cause chronic symptoms, such as pain and fatigue. However, there are crucial differences.
Multiple sclerosis (MS) is a neurological condition. It causes the immune system to attack the central nervous system and damage the nerves’ protective coating, which is called myelin.
Fibromyalgia is a complex condition that affects many of the body’s functions. The most telltale symptom is widespread pain and tenderness in the muscles and joints. Unlike MS, fibromyalgia is not an autoimmune disease.
Currently, the medical community does not fully understand what causes fibromyalgia. The symptoms appear to result from the central nervous system sending the wrong signals to the brain.
In this article, learn about the differences between MS and fibromyalgia and how doctors diagnose and treat these conditions.
MS vs. fibromyalgia symptoms
Fibromyalgia and MS share some symptoms, such as muscle weakness and pain. However, there are key differences, including the types of pain and accompanying issues:
Fibromyalgia pain
Fibromyalgia can cause body aches and pains.
Fibromyalgia pain is typically widespread and lasts a long time.
The skin may always feel tender, and some areas may be more sensitive than others.
People with fibromyalgia often describe the pain as dull, achy, and persistent.
Fibromyalgia pain often occurs on both sides of the body and in areas above and below the waist.
For a diagnosis of fibromyalgia, the pain must have lasted for at least 3 months.
Other fibromyalgia symptoms
Other symptoms of fibromyalgia include:
- Fatigue: Fibromyalgia typically causes chronic fatigue. People with the condition may need to take long breaks between activities or get extra sleep.
- Restlessness: Some people experience restlessness or restless legs syndrome. They may have a hard time getting comfortable or relaxing, and they may develop sleep disturbances, such as insomnia.
- Fibro fog: This term describes a lasting sense of confusion or difficulty concentrating that results from fibromyalgia. Some research suggests that it occurs because the brain is trying to tune out pain, which makes thinking more difficult.
MS pain
MS affects nerves throughout the body. Damaged nerves may fire without cause, leading to pain and other sensations in one or multiple areas.
The pain affects people differently, but some describe it as:
- a stinging sensation beneath the skin
- a feeling of numbness, as though certain areas are “falling asleep”
- uncomfortable tingling
- pins and needles
- a sensation of electricity
The severity can vary, depending on how far MS has progressed. Some people only experience tingling, while others experience widespread, debilitating pain.
Other symptoms of MS include:
Changes in speech: As the immune system damages the nerves, it can take more time for signals to reach the brain. This can make speech slow or difficult.
Vision changes: Nerve damage can also affect the eyes, leading to blurred or double vision. Some people experience extensive or complete vision loss.
Difficulty moving or walking: Nerve damage can lead to muscle weakness in the arms or legs, which can affect the way a person walks. Their gait may become disrupted or unsteady.
Coordination: Damage to the nerves can also inhibit a person’s coordination, causing them to feel off-balance or dizzy.
Bladder and bowel changes: People with MS may need to urinate or have bowel movements more frequently, for example.
Diagnosis
A doctor may use a blood test to help diagnose chronic conditions.
Diagnosing either condition can be challenging, and it may involve a process of elimination.
If a doctor suspects that a person has MS, they will often use an MRI to check for damage to the brain and spinal cord.
If they are still unsure, they may request a lumbar puncture, which involves removing some fluid from the spine and checking it for antibodies that occur in cases of MS.
This is the most accurate way to diagnose the condition.
There is no single test for fibromyalgia, and a doctor may first need to rule out other explanations for symptoms.
Nerve conduction tests, electromyograms, skin biopsies, and blood tests are common methods that doctors use when diagnosing the condition. A doctor may also ask how small pains feel because they tend to hurt more in people with fibromyalgia.
The doctor may also investigate any tender points on the body. These are areas that are especially sensitive in people with fibromyalgia.
Life expectancies
MS and fibromyalgia are long-term conditions, but neither is life-threatening.
The National Multiple Sclerosis Society suggest that MS may reduce a person’s lifespan by 7 years, and that severe and rapidly progressing forms can be fatal.
The National Institute for Neurological Diseases and Stroke suggest that a person with MS will have the same life expectancy as a person without the disease.
Symptoms of fibromyalgia can be persistent, while those of MS can progress and become debilitating.
Treatments
As there is no cure for either condition, treatments involve managing and reducing symptoms to improve the quality of life.
MS treatment
Having a thorough treatment plan can help relieve symptoms, prevent flare-ups, and slow the progression of the condition.
An emerging class of drugs called disease-modifying therapies can help reduce the number of flares and may also slow progression.
Other treatment, such as corticosteroids, can help manage flares and the symptoms that can arise.
Some over-the-counter medications can provide temporary relief from symptoms such as pain. Options include:
- ibuprofen (Advil)
- acetaminophen (Tylenol)
- aspirin (Bayer)
A doctor may prescribe the following for pain and itching:
- hydroxyzine (Atarax)
- phenytoin (Dilantin)
- amitriptyline (Elavil)
- clonazepam (Klonopin)
- gabapentin (Neurontin)
- nortriptyline (Pamelor, Aventyl)
- carbamazepine (Tegetrol)
Alternative therapies that may also help include:
- techniques to relieve stress, such as breathing exercises and meditation
- low-impact activities, such as swimming, tai chi, and yoga
- acupuncture
- reflexology
However, there is not enough evidence to confirm that all of these are useful for people with MS.
Fibromyalgia treatment
Regular aerobic exercise can help treat fibromyalgia.
The National Fibromyalgia & Chronic Pain Association states that the following can help people manage the condition:
- Education: Doctors should provide information about the condition and various treatment options. Some people find that researching independently helps them find better treatments and more relief.
- Aerobic exercise: It may help to follow an exercise routine every day. This does not need to be strenuous but should get the heart rate up.
- Mental health support: Tools such as cognitive behavioral therapy may complement treatment. Also, support from friends, family, and groups can be crucial for a person’s overall well-being.
- Medicinal therapy: Some prescription drugs can reduce symptoms such as pain.
As there are not many direct medical treatments for the condition, complementary therapies may be a good option. These include:
- physical therapy
- myofascial tissue release
- chiropractic manipulation
- hot and cold therapy
- massage
- acupuncture
- relaxation techniques
- yoga
- aromatherapy
- herbs and supplements
What else could it be?
Fibromyalgia and MS can be challenging to diagnose because their symptoms resemble those of many other conditions, including:
- chronic migraines
- lupus
- rheumatoid arthritis
- sarcoidosis
- neuromyelitis optica spectrum disorder
- Lyme disease
- myasthenia gravis
- Sjogren’s syndrome
- neuropathy
Conclusion
MS and fibromyalgia are different conditions that can cause similar symptoms. There is no cure for either condition, but there are many methods of managing symptoms.
Speak to a doctor about any undiagnosed symptoms and work with them to develop a comprehensive treatment strategy.